Stumpy the Blue-Tongued Skink receives Red Light Therapy
Recently, Tony Nevin or Zoo Ost Ltd (link) found himself caring for two blue-tongued skinks who came to him for rehabilitation, during which they had a session of sibling fisticuffs and Stumpy sustained an injury. Tony used a combination of osteopathic methods and Photizo red light therapy to assist in Stumpy’s recovery.
Bumblefoot in Penguins
Bumblefoot, also known as ulcerative pododermatitis, is a common bacterial infection that occurs on the feet of penguins as well as other birds and animals. The bacteria naturally occurs in the animal’s environment and infection breaks out when there is a scrape or cut in the skin. Despite it’s quirky name, Bumblefoot can be fatal if left untreated. Warning signs include limping, lopsided posture and lying down for extended periods of time.
Red Light Therapy for Plantar Fasciitis
Have you ever experienced plantar fasciitis? This blog explains what plantar fasciitis is, how to recognise the symptoms, what causes plantar fasciitis, the commonly recommended self-help treatments, and how Red Light Therapy (also known as photobiomodulation) can help relieve the pain and inflammation to accelerate recovers from this debilitating injury.
Red Light Therapy and Thyroid Health
In the pursuit of holistic well-being, emerging wellness modalities like red light therapy, also known as photobiomodulation (PBM), have gained attention for their diverse benefits. In this blog, we ask the question – does red light therapy offer benefits for thyroid conditions? Or should it be avoided?
Harnessing the Power of Red Light Therapy for Arthritic Hands: A Gentle Approach to Relief
Living with arthritic hands can be a daily challenge, impacting not only our physical abilities but also our overall well-being. The two most common types of arthritis are osteoarthritis and rheumatoid arthritis. Osteoarthritis is a degenerative joint disease that is characterised by progressive and uneven loss of articular cartilage, bone spurs, and hardening of the underlying bone, as well as other abnormalities. Rheumatoid arthritis is a chronic autoimmune disease. Both are more common in women. The current treatment offered is commonly prescription medication which may have side effects. The search for effective and gentle relief has led many individuals to explore alternative therapies such as red light therapy, also known as photobiomodulation, or PBM for short. In this blog, we'll delve into the potential benefits of red light therapy for arthritic hands, supported by studies that highlight its positive effects.
Joker, Siberian Husky Puppy - healing journey from broken femur to adult Racing Husky
Joker, the 7 month old Siberian Husky Puppy - healing journey using Photizo Vetcare and Leucillin.
After a freak accident whilst playing with his brother in the garden on 5th June 2022, 7-month old Siberian Husky puppy, Joker broke his back left leg and sustained a spiral fracture to his femur which was close to both joints.
Learn how Joken recovered from broken femur to adult Racing Husky Working Dog.
Team Photizo supporting the 40th and Final Aviemore Sled Dog Rally
Every year since 1984, mushers from the UK have gathered in the forests around Aviemore for the biggest event in the British sled dog racing calendar, The Siberian Husky Club of Great Britain Aviemore Sled Dog Rally January 27th-28th will be the 40th anniversary rally and also the last ever SHCGB Aviemore Rally. Team Photizo have been a proud joint sponsor with CSJ and Leucillin for several years and we’ve had the most incredible experience at this memorable prestigious mushing event in the UK sled dog racing calendar.
An integrated natural healthcare solution to re-balance Ruby, the Cockapoo
When Liz Turner reached out about Ruby, a 6 year old Cockapoo, she had a few issues, including recurring cystitis. She also had some digestive reflux problems and was quite anxious with respect to sounds. Ruby had begun some ‘fly-catching’ behaviour, (gasping at the air as though catching imaginary flies), which is very distressing.
How Does Red Light Therapy Work?
What is Red Light Therapy (also known as Photobiomodulation), how does it work and how can it help me? Your questions summed up…
Red Light Therapy for Female Health
Whether you’re struggling with menstrual cramps, post-partum pains, skin issues or menopause symptoms, PBM may be a much needed relief. Here is how…
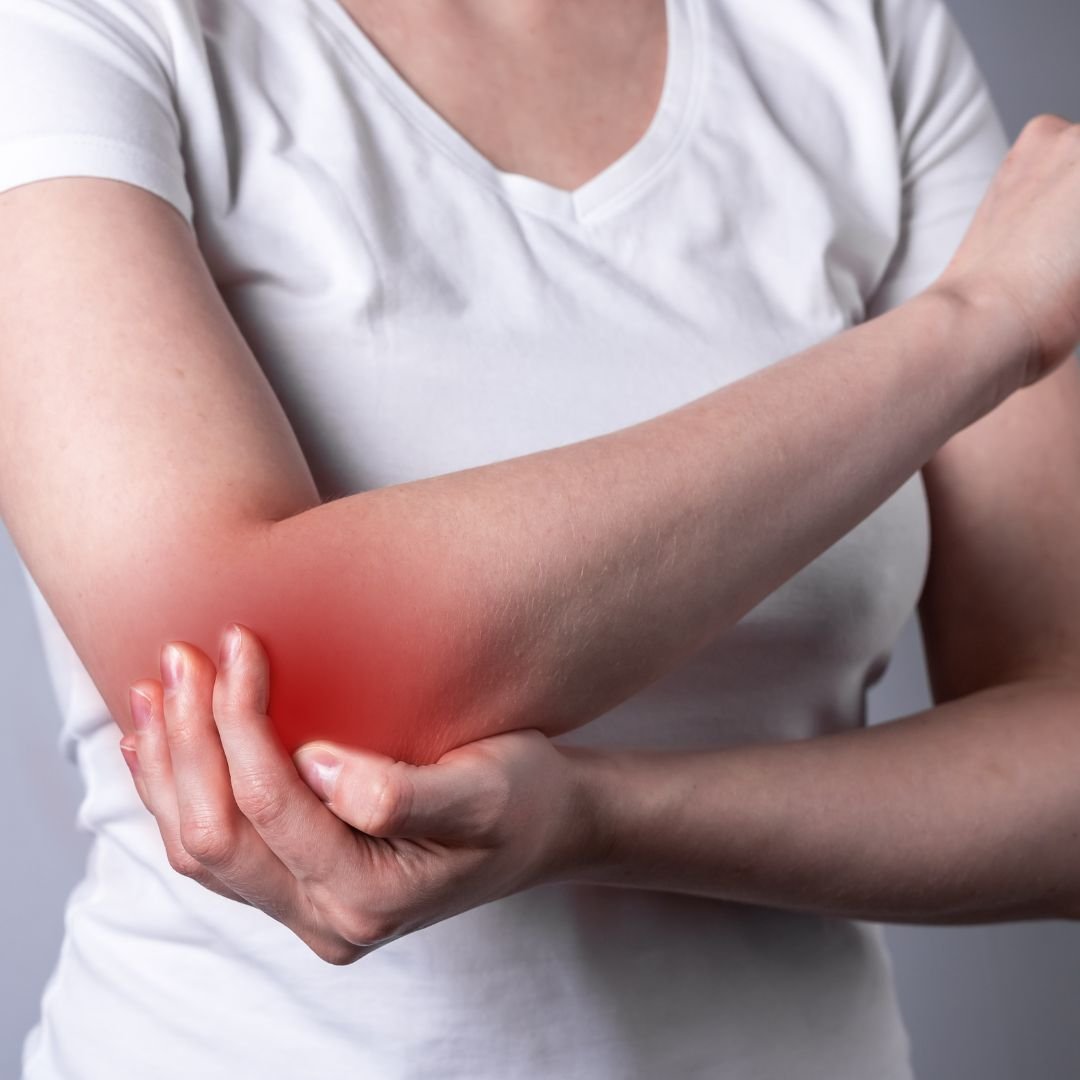
Red Light Therapy for Tennis Elbow and Golfer’s Elbow
You don’t have to be a tennis player or a keen golfer to experience these extremely painful conditions.
Inky’s Journey: A SNORS story
The little rabbit saved by a charity with a big heart. Despite Inky’s health issues, where some would have given up, he was saved by love.
Illuminating the Past: A Journey into Light Healing
The history of using light as medicine, and how we have come to use Photobiomodulation as a healing modality.
BobDog, The Adorable RUFFian
The story of a little furry thief was sent across to us at Photizo HQ. The tale of an adorable pooch, an unlikely suspect…